Pain is the most complex human experience. But is it only physical? Why does heartbreak ache when there’s no wound, yet a soldier in the heat of battle barely feels pain despite of both physical and emotional injury? If pain is created by the brain interpreting signals, what does that say about its purpose, and why does the Qur’an speak of replacing skin so that pain is fully experienced in the hereafter? Let’s answer all these questions.
Blog Summary:
- What is Pain? A Human and Scientific Understanding
- Etymology
- Pain is Not Just Physical: A Real-Life Example
- The Science Behind Pain: Nociception vs Pain
What is Pain? A Human and Scientific Understanding
Pain is one of the most universal experiences in human life. Every human being encounters it at some point, yet when we try to explain what pain actually is, the answer becomes surprisingly complicated. At first, pain seems simple: something hurts, and we feel it. However, modern science shows that pain is not just a physical sensation caused by injury. Instead, it is a complex experience created by the brain, involving the body, the mind, emotions, and even our personal experiences.1
Etymology
The word “pain” originates from the Latin poena, meaning “punishment” or “penalty,” tracing back through Old French peine and Greek poinē, meaning “a price paid.”2
Pain is Not Just Physical: A Real-Life Example
A powerful example helps us understand this. In 1995, doctors described a case of a construction worker who jumped onto a long nail. The nail appeared to go straight through his boot, and he was in extreme pain. Even the smallest movement caused him agony, and he had to be taken to the hospital. Doctors expected a serious injury. But when they removed his boot, something surprising happened, the nail had passed between his toes without touching his foot at all.There was no injury. Yet the pain he felt was completely real.3
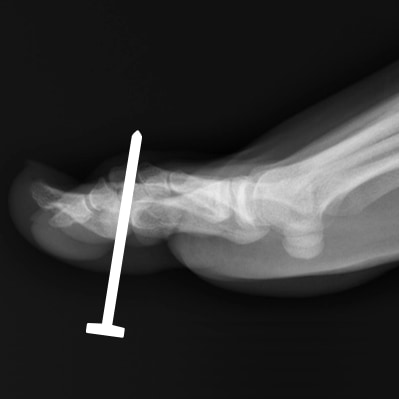
This case shows something very important: pain is not just about physical damage. It is something the brain creates based on what it believes is happening. The brain saw the situation, predicted danger, and produced pain as a protective response.
The Science Behind suffering
To understand this better, scientists separate two ideas: nociception and pain. Nociception is the physical detection of harmful or potentially damaging stimuli in the body. Special nerve endings, called nociceptors, are located in the skin, muscles, joints, and organs, and they respond to things like heat, pressure, chemical irritation, or tissue injury. When these nociceptors are activated, they send electrical signals to the spinal cord and brain.4
Pain is what we actually experience consciously. It is the brain’s interpretation of these signals, combining biological input with context, emotions, and memory5.Biologically, pain is not just a feeling, it triggers a cascade of protective responses in the body. For example, when nociceptors detect a harmful stimulus, the brain may:
- Increase heart rate and blood pressure to prepare the body for action
- Dilate pupils to improve visual awareness
- Release prostaglandins and other inflammatory mediators, which amplify the pain signal and help the body respond to injury
These biological responses illustrate that pain is both a warning system and a coordinated physiological process designed to protect us from harm.6
Brain itself has no nociceptors
Interestingly, the brain itself does not contain nociceptors, which is why surgeons can operate on brain tissue while patients are awake without causing direct pain . So why do we feel headaches, migraines, or other brain-centered pain?The answer lies in the nociceptors located in blood vessels, meninges, and surrounding tissues around the brain. The brain interprets signals from these areas as pain, generating the experience of headaches even though the brain tissue itself cannot feel pain.7
In this sense, pain is biologically real and protective, but it is always a creation of the brain, shaped by both body signals and neural interpretation. It is the ultimate example of how biology and perception work together to keep us safe and aware of danger.
Emotional Suffering is also Real
Pain is not only physical, it is also deeply emotional. Research by Eisenberger and Lieberman (2004)8 showed that emotional pain, such as heartbreak or rejection, activates the same areas of the brain as physical pain. In their study, people who had experienced a breakup felt real pain just by looking at photos of their former partners. This shows that pain is not something we simply “feel” in the body, it is something we live through in the mind and heart.
Anyone who has experienced loss knows this feeling. There is no visible wound, no bleeding, yet the pain can feel just as sharp as a physical injury. A memory, a voice, or even a photograph can bring back a wave of heaviness in the chest, a tightness in the throat, or an ache that is hard to explain. The brain does not clearly separate emotional suffering from physical harm; instead, it responds as if both are equally significant.9
This is what makes pain so deeply human. It is shaped by our relationships, our memories, and the meaning we attach to experiences. Two people can go through the same situation, yet feel completely different levels of pain because their emotional worlds are different. In this way, pain becomes more than just a biological signal, it becomes a story of connection, loss, and vulnerability.
Understanding this reminds us to treat pain with compassion. Just because we cannot see someone’s suffering does not mean it is not real. Emotional pain deserves the same care and attention as physical pain, because for the person experiencing it, the hurt is just as powerful, just as real, and sometimes even harder to heal.
The Shared Pathways
And this is where a key connection emerges: the same brain regions that process physical injury also generate emotional or psychological pain. Because of this shared system, individuals who are more sensitive to physical pain often tend to be more sensitive to emotional pain as well. 10
Suffering as a Protective System
From an evolutionary point of view, suffering, distress, ache are actually helpful. It works like an alarm system that protects us from harm. If you touch something hot, agony immediately makes you pull your hand away. If you break a bone, suffering forces you to slow down, rest, and allow the body to heal properly. In this way, pain acts as a built-in survival mechanism, guiding behavior and keeping us safe from further injury.1112
Congenital Insensitivity
This protective role becomes even clearer when we look at people with Congenital Insensitivity to Pain (CIP)13, a rare condition in which individuals cannot feel pain. While it might sound like an advantage, it is extremely dangerous. Pain is a vital signal that helps people avoid danger and injuries. People who cannot feel pain experience more injuries and may have shorter life expectancies.14 People with CIP often suffer repeated injuries, burns, or broken bones without noticing. They may bite their tongues or fingers, walk on fractured limbs, or touch hot surfaces, all without the warning signals that pain normally provides. Over time, these unnoticed injuries can lead to infections, joint damage, and serious complications, sometimes even threatening life.
Our natural Teacher
Agony also shapes learning and behavior in subtle ways. From a young age, it teaches us to avoid dangerous situations, like touching fire, climbing unstable heights, or running into traffic. Even minor pains, such as stubbing a toe or scraping a knee, leave lasting memories that guide future actions. In this sense, pain is not merely unpleasant; it is a teacher, a guide, and a silent guardian, constantly working to protect our bodies and our lives. And this is one way to answer of another question: If God is all-merciful, why there is so much suffering?
Different Types
Pain can thus appear in different forms which are as given below:
| Acute – Short-term, signals from injury or illness (e.g., a cut, burn, or surgery). |
| Chronic – Long-lasting, usually persisting beyond normal healing (e.g., arthritis, back pain). |
| Neuropathic – caused by nerve damage or dysfunction (e.g., sciatica, diabetic neuropathy). |
| Nociceptive – From actual or potential tissue damage, sensed by pain receptors (can be somatic or visceral). |
| Psychogenic or emotional – Influenced by emotional, psychological, or social factors (e.g., grief, social rejection). |
The Brain Predicts: Predictive Coding
Modern neuroscience introduces the idea of predictive coding15, which suggests that the brain is constantly trying to anticipate what will happen next. It builds an internal model of the world and uses past experiences to predict danger, discomfort, or injury. If the brain expects harm, it can generate discomfort even when there is no real injury, as a protective mechanism. This explains why sometimes we “feel” pain long after an injury has healed.
Pavlov’s Contribution
For example, imagine someone who once hurt their back while bending. Even after the bones and muscles have fully healed, the brain may continue to produce pain whenever they bend again. The mind remembers the previous injury, and the body reacts as if the danger is still present. This learned response is similar to conditioning, a principle famously described by Pavlov (1927). Over time, the neural circuits that fire in response to bending are strengthened, so the brain begins to predict pain automatically, even without any tissue damage.
Memory of Pain
Pavlov’s experiments on classical conditioning showed that a neutral stimulus, like a bell, can trigger a learned response, such as salivation, when repeatedly paired with an unconditioned stimulus, like food. Similarly, in chronic pain, the brain can “learn” to expect pain even after an injury has healed. For example, bending after a back injury may automatically trigger pain because the neural circuits have been conditioned to predict it, illustrating how past experiences shape our body’s responses.

Healing is not always about fixing the body alone
Understanding predictive coding helps explain why healing pain is not always about fixing the body alone. The mind and emotions must also be addressed, because the brain’s predictions are deeply connected to our feelings and experiences. Pain, in this sense, is as much psychological and emotional as it is biological, it is a full-body experience that blends memory, fear, and hope with the physical signals from the body.
Psychological and Social Influences on Pain
Pain is not just a physical sensation; it is deeply influenced by our thoughts, emotions, and environment. Stress, fear, and anxiety can amplify the intensity of pain, making even minor injuries feel unbearable. On the other hand, feelings of safety, comfort, or distraction can reduce pain, demonstrating how closely our mind and body are intertwined in shaping the experience of suffering.
During World War II, physician Henry Beecher (1946) observed a remarkable phenomenon: injured soldiers often reported less pain on the battlefield than they did afterward. Despite severe wounds, their focus on survival and the urgency of combat seemed to temporarily suppress their pain. Once the immediate danger passed, the pain became more noticeable. This shows that attention, context, and emotional state can directly alter how pain is perceived, highlighting the brain’s central role in creating the experience of suffering.
Pain is also social and relational. Humans are capable of experiencing what neuroscientists call empathic pain—the distress we feel when witnessing the suffering of others. When we see someone injured or in emotional turmoil, the brain activates some of the same regions involved in our own pain (Singer et al., 2004). This ability forms the biological foundation for empathy, compassion, and social connection, reminding us that pain is not only a personal signal but also a bridge that connects us to other people’s experiences.
Moreover, pain can shape relationships and moral awareness. For example, seeing a loved one suffer can inspire protective behavior, strengthen bonds, and guide ethical decisions. In this sense, pain is not just an unpleasant sensation—it is a teacher of resilience, empathy, and human connection, demonstrating how deeply our physical and emotional worlds are intertwined.
Right now, pain is more complex than ever we might imagine. It is not just a signal from a broken bone or a cut; it can arise from emotional wounds, psychological distress, or even the anticipation of danger. Pain can exist even when there is no visible injury, and sometimes it disappears in moments of extreme survival. Imagine you are running from a dog, and in the chaos, your leg is fractured—but you don’t feel the pain at that moment. The body prioritizes survival, and the brain temporarily suppresses the signals.
Over time, repeated pain can reshape the brain itself through neuroplasticity. The neurons “learn” the pain, making it part of the body’s predictive system. Chronic pain can become habitual; the brain expects it, amplifies it, and the person carries it as a constant companion. It becomes part of their lived experience. As the great Urdu poet Mirza Ghalib beautifully expressed:
رنج سے خوگر ہوا انساں تو مٹ جاتا ہے رنج
مشکلیں مجھ پر پڑیں اتنی کہ آساں ہو گئیں
Translation:
When man becomes accustomed to pain, then the pain vanishes;
So many difficulties fell upon me, that they became easy.
This line captures the profound human truth that pain, in its many forms, physical, emotional, or psychological, can become woven into the fabric of our lives. It is a teacher, a warning, and sometimes, a companion that shapes not only our body but also our heart and mind.
The Human Body and the Urgency of Pain
When we reflect on the human body through both science and faith, as highlighted in the Qur’an, which states that الإنسان is created in the best form, one system that immediately stands out is the system of pain. Now, let me put this to you as I would in a conversation: have you ever wondered why pain feels so immediate, so raw, and so impossible to ignore? The answer lies in how pain receptors—nociceptors—are designed. Unlike other sensory receptors, these are free nerve endings, meaning they are unencapsulated, undifferentiated, almost “naked” nerve terminals. And that simplicity is not accidental; it is essential. These receptors are not built to analyze or interpret—they are built to warn, and to warn fast.
Free Nerve Endings and the Need for Speed
Think about it this way: if you move your hand toward fire, your body does not pause to evaluate, analyze, or debate whether the heat is dangerous. It reacts instantly. Why? Because nociceptors do not involve themselves in complex preprocessing. Their structure allows them to detect harmful stimuli and immediately convert it into electrical signals. These signals travel through fast A-delta fibers and slower C fibers, and in many cases, your spinal cord triggers a withdrawal reflex before your brain even becomes consciously aware of the pain. This is a system designed for survival, not comfort. Encapsulated receptors—those responsible for fine touch or vibration—take time to process detailed information. Pain receptors, on the other hand, bypass that luxury because delay could mean damage.
A Wide Range of Painful Stimuli
Now you might ask, how can one type of receptor deal with something as broad as pain? After all, pain can come from heat, pressure, chemicals, or injury. The answer is that nociceptors are capable of detecting multiple forms of harmful stimuli. Some respond specifically to extreme temperatures, others to mechanical damage like cuts or pressure, and others to chemical signals released during tissue injury. Many are polymodal, meaning they can respond to several types of stimuli at once. But here is the important distinction: not every touch, temperature, or pressure is pain. These sensations only become pain when they cross a certain biological limit—when they reach a level that threatens tissue integrity.
Nociceptors Receptors: High-Threshold Sensors for Survival
When we think about pain, it’s easy to imagine that pain receptors are somehow “supercharged” neurons with a higher electrical threshold than other nerve cells—but that’s not exactly correct. In reality, nociceptors function like all neurons electrically: their threshold potential—the level of depolarization needed to fire an action potential—is similar to that of other neurons. What sets them apart is their high stimulus threshold. This means they only respond when a stimulus is strong enough to potentially damage tissue, whether it’s extreme heat, intense pressure, chemical injury, or severe mechanical stress. Normal touch, gentle warmth, or light pressure does not activate them. This design makes perfect sense: if pain receptors responded to every minor sensation, we would feel constant pain from harmless daily activities. Instead, the body separates sensation into low-threshold receptors, which detect normal touch, vibration, and mild temperature, and high-threshold nociceptors, which act as emergency alarms, activating only when danger arises. Because of this, pain signals are rapid, direct, and hard to ignore, allowing the body to respond instantly—like pulling your hand away from fire—without waiting for detailed processing. In short, nociceptors are not “electrically stronger” neurons; they are finely tuned sensors that prioritize survival by responding only when truly necessary.
Why Simplicity is Perfection
So if I were to ask you: why are pain receptors so simple compared to others? The answer becomes clear. Complexity would slow them down. Encapsulation and specialization are useful when the body needs detailed information, but pain is not about detail—it is about urgency. Free nerve endings allow direct, rapid signaling without delay, ensuring that the body responds immediately to threats. This simplicity is, in fact, a form of precision.
Nociceptors Receptors, the Skin, and the Verse in the Holy Qur’an
In the human body, pain receptors—scientifically called nociceptors—are found throughout the skin and deeper tissues. These receptors are free, unencapsulated nerve endings that respond only when stimuli are strong enough to threaten tissue integrity, such as extreme temperature, intense pressure, or chemical injury. They are high‑threshold sensors designed to activate only under harmful conditions so that the body can react immediately without delay; this is why you instinctively withdraw your hand from heat before your brain has fully processed the danger. Their structure and function are described in standard physiology texts, which explain that normal touch and mild sensations do not activate these receptors—only potentially damaging stimuli do.
The skin is the largest sensory organ of the body and one of the richest in nociceptors, especially those that detect heat and mechanical injury. There are nociceptors associated with somatic (skin and musculoskeletal) structures and those associated with visceral (internal organ) structures, each tuned to the kind of harmful stimulus relevant to its location. This distribution ensures that the body detects external threats as well as internal injury.
Interestingly, the Qur’an contains a verse that emphasizes the role of the skin in sensation and pain, stating: “Indeed, those who disbelieve in Our verses—We will drive them into a Fire. Every time their skins are roasted through, We will replace them with other skins so that they may taste the punishment. Indeed, Allah is Almighty, All‑Wise.” (Surah An‑Nisa 4:56).
This verse refers to the replacement of skin repeatedly so that the punishment—and the pain associated with it—can continue. From a scientific perspective, the sensation of temperature and pain is directly linked to receptors in the skin; without functioning skin and nociceptors, a person would not feel those sensations. When skin is destroyed by extreme heat, the peripheral nerve endings that mediate pain are also destroyed, and pain sensation ceases in the damaged area. The biological necessity for intact nerve endings to feel pain aligns with the implication of the Qur’anic verse: that if the skin and its receptors were gone, the sensation of pain would no longer occur, and therefore they would be replaced so that the painful experience continues.
Although specific historical documentation of scientists like Professor Tagatat Tejasen publicly linking this verse to modern neuroscience is limited in peer‑reviewed literature, it is true within neurobiology that the skin contains an abundance of nociceptors and that these receptors are essential for detecting external harmful stimuli and generating pain signals to the central nervous system. This scientific understanding helps clarify why the Qur’anic verse specifically mentions the skin as the locus of repeated sensation.
References
- In 2020, the International Association for the Study of Pain (IASP) updated the definition of pain as “an unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage.” This definition highlights that pain is multidimensional, involving sensory, emotional, and cognitive components. It includes both nociceptive pain, arising from actual harmful stimuli, and neuropathic or spontaneous pain, which can occur without tissue damage. ↩︎
- https://en.wikipedia.org/wiki/Pain ↩︎
- The “Boot Nail Guy” story originates from a 1995 report in the British Medical Journal’s Minerva column. https://www.painscience.com/blog/legend-of-boot-nail-guy.html
While the incident likely occurred, the report was anecdotal, not a formal case study, and many details remain uncertain. The case is widely cited in pain science as an illustration of how pain perception can be strongly influenced by the mind, including fear and anxiety, demonstrating that pain is not solely a direct response to tissue damage but is modulated by the brain. ↩︎ - Nociception is not equivalent to pain https://pain.ucsf.edu/understanding-pain-pain-basics/nociception-versus-pain ↩︎
- Advances in neuroimaging have greatly improved our understanding of how the brain processes pain, showing that perception is influenced by multiple factors such as cognition, emotion, context, and injury. https://pubmed.ncbi.nlm.nih.gov/17678852/ ↩︎
- Modern research shows that pain is not just processed at the site of injury but is heavily shaped by higher brain (supraspinal) mechanisms. These brain processes play a major role in how pain is experienced, why it differs between individuals, and how it can lead to chronic disability.https://pubmed.ncbi.nlm.nih.gov/15979027/ ↩︎
- If the brain can’t feel pain, why do I get headaches?
https://www.brainfacts.org/ask-an-expert/if-the-brain-cant-feel-pain-why-do-i-get-headaches ↩︎ - Pain overlap theory proposes that social pain, the pain that we experience when
social relationships are damaged or lost, and physical pain, the pain that we
experience upon physical injury, share parts of the same underlying processing
system https://sanlab.psych.ucla.edu/wp-content/uploads/sites/31/2015/05/Eisenberger_ch7-2005.pdf ↩︎ - Scientific research supports this idea, showing that social and physical pain share overlapping brain mechanisms. https://pubmed.ncbi.nlm.nih.gov/15242688/ ↩︎
- HYPOTHESIS #4: TRAIT DIFFERENCES RELATING TO ONE TYPE OF PAIN RELATE TO THE OTHER TYPE AS WELL. Page 13 https://sanlab.psych.ucla.edu/wpcontent/uploads/sites/31/2015/05/Eisenberger_ch7-2005.pdf ↩︎
- The Physiology of Pain
https://www.physiology.org/publications/news/the-physiologist-magazine/2022/march/the-physiology-of-pain?SSO=Y ↩︎ - https://www.ncbi.nlm.nih.gov/medgen/344563?utm ↩︎
- Congenital insensitivity to pain (CIP), also known as congenital analgesia, is an inability for a person to feel physical pain due to various rare genetic conditions. https://en.wikipedia.org/wiki/Congenital_insensitivity_to_pain ↩︎
- https://www.ncbi.nlm.nih.gov/medgen/344563?utm ↩︎
- Predictive coding, also called predictive processing, is a neuroscience theory proposing that the brain constantly generates and updates a mental model of the environment to predict incoming sensory signals. These predictions are compared with actual sensory input, and any mismatch (prediction error) is used to update the model. https://en.wikipedia.org/wiki/Predictive_coding ↩︎
Discover more from Ayhian Ali 🦖
Subscribe to get the latest posts sent to your email.